Diabetes is a serious global illness that is only getting worse. Globally, the occurrence of diabetes among people over 18 years of age has grown from 4.7% in 1980, to 8.5% in 2014. The World Health Organization has estimated that diabetes is the seventh-leading cause of death worldwide.
What is diabetes?
Insulin is a hormone, produced by the pancreas. Our bodies need insulin to regulate blood sugar. For people with diabetes, their pancreas either cannot produce enough insulin, or cannot actually use the insulin that is produced. The result is hyperglycemia, or raised blood sugar, which can lead to serious damage to the body, and particularly the nervous system and blood vessels.
Why is it important to monitor blood sugar?
For those suffering from diabetes, monitoring blood sugar is essential. By knowing their blood sugar, diabetics can:
- Gauge how well their current treatment and medication regimen is progressing.
- Understand the impact of diet, exercise, illness, stress, and other stimuli on their diabetes.
- Take action if their blood sugar levels become very high or very low.
How is blood sugar monitored?
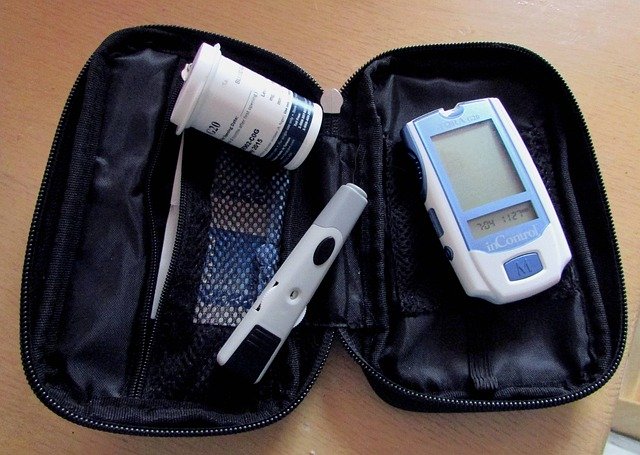
Blood sugar is monitored using a meter. There are three different types of meters:
Blood glucose meter
This is the most common type of meter used to measure blood sugar and remains the industry standard for monitoring. Its use involves inserting a strip into the meter, pricking one’s fingertip with a lancet, and collecting the blood onto the strip. The meter then reads the strip. Blood glucose meters are generally accurate when used and maintained properly.
Alternative site/flash glucose monitor
These meters are a newer type of device that do away with finger pricking, instead of using sensors to measure blood sugar. The sensor is inserted just underneath the skin (usually the upper arm), and a hand-held scanner is swiped over the sensor to read the blood sugar level. These monitors are not as accurate as traditional blood glucose monitors.
Continuous glucose monitor (CGM)
Also using a sensor inserted underneath the skin, these monitors check blood sugar continuously throughout the day. Alarms go off if blood sugar is high or low, and the monitor is integrated with an insulin pump. However, these monitors are expensive, as the sensors need to be replaced every 3-7 days, and the user must still employ a traditional blood glucose monitor to confirm the CGM measurement, and to program the monitor.
Top things to look for in a blood glucose monitor
When considering a blood glucose monitor, many factors need to be taken into account, such as:
- Cost: this includes not only the cost of the monitor itself but also the cost of the accompanying test strips.
- Ease of use: consider not only how easy a meter is to use, but how easy it is to read.
- Data storage and retrieval: check to see how much information is stored with each reading that is taken. For example, some meters include the time and date of the reading, while some can also show trends over time. Some can also download data to a computer or mobile device, or send the results to a physician.
- Insurance coverage: some insurance companies only cover specific monitors or have a limit on the number of test strips that can be purchased under coverage.
- Special features: some of these include large buttons, audio prompts (for diabetes sufferers with reduced vision), and illuminated displays.
- Support: look for elements such as a toll-free support phone number (as well as the hours that support staff are available to talk), online manuals, etc.
Written by Raymond Quan
References:
Comparative accuracy of 17 point of care glucose monitors
Image by Pamula REEVES-BARKER from Pixabay